Cosmetic Surgery Blog
Good and Bad news for patients with lots of moles
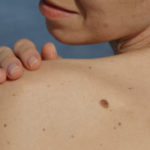
A recent study confirms that patients with lots of moles (more than 50) and patients with dysplastic (atypical) moles are at higher risk for melanoma and develop their melanomas at a younger age. However the good news is that these same patients seem to have their melanomas diagnosed earlier and at a less aggressive stage than patients with fewer moles. This is at least partly due to more careful and regular skin cancer surveillance in the “high risk” group. One important lesson from this study is everyone needs to regularly check their moles. Higher risk patients (those with lots of moles and atypical moles) because they are more likely to develop melanoma, and lower risk patients (those with fewer and more typical moles) to avoid latter diagnosis of the melanomas they do develop.
Citation:
Association of Clinicopathological Features of Melanoma With Total Naevus Count and a History of Dysplastic Naevi: A Cross-Sectional Retrospective Study Within an Academic Centre
Clin Exp Dermatol 2018 Jul 01;43(5)566-572, SY Tan, LC Strazzulla, X Li, JJ Park, SJ Lee, CC Kim
More on Melanoma
The bugs living in your guts might save you!

The importance of which specific bugs you have in your body, your “microbiome” , is becoming increasingly recognized. Now a study has show that patients’ repose to an immune therapy used in advanced melanoma, varied based on their specific microbiome. Investigators used stool samples to get an accurate picture of each patients microbiome before treatment with anti-PD-1 therapy for advanced melanoma. They found a strong correlation between specific bugs in patients’ microbiome and their response to therapy. Further more, microbial reconstitution of germ-free mice with fecal material from responding patients improved tumor control and augmented T-cell responses in mice. It is logical to hope that adjusting human microbimes prior to therapy will improve their subsequent response to this and potential other treatments.
Citation:
The Commensal Microbiome Is Associated With Anti-PD-1 Efficacy in Metastatic Melanoma Patients
Science 2018 Jan 05;359(6371)104-108, V Matson, J Fessler, R Bao, T Chongsuwat, Y Zha, ML Alegre, JJ Luke, TF Gajewski
Eyes and Melanoma

Take a closer look at your eyes. What can your eyes tell you about your melanoma risk? Well we already know that people with light colored eyes, blue or green tend to have a higher risk of skin cancer in general. A recent study has shown that pigmented lesions on the iris (that’s the colored part of your eye) may be a risk factor for skin melanoma in patients under 40 years old. The presence of three or more iris pigmented lesions resulted in a 1.80-fold increase risk for melanoma in participants younger than 40 years. These results suggest that iris pigmented lesions can serve as a marker for younger people at higher risk for melanoma. The risk increases proportionally to number of iris lesions.
Article Citation:
The British Journal of Dermatology
Iris Pigmented Lesions as a Marker of Cutaneous Melanoma Risk: An Australian Case-Control Study
Br J Dermatol 2018 Jan 08;[EPub Ahead of Print], AM Laino, EG Berry, K Jagirdar, KJ Lee, DL Duffy, HP Soyer, RA Sturm
Meat and Melanoma

Maybe red meat is not all bad! A recent study looked for a link between consumption of red and processed meat and melanoma. They used data from over 75,000 women and 48,000 men from the Nurse Health Study and Health Professionals follow up Study. In these groups a total of 1318 melanomas were identified. I am sure the investigators were expecting to show red meat is bad and dangerous. Surprisingly, red and processed meat intake was inversely associated with melanoma risk. That means that people who eat more red and processed meat had a slightly lower risk of melanoma! While this may be due to some other “associated behavior”, (maybe meat eaters are spending less time in the sun), we should not ignore the result just because it doesn’t fit into our paradigm of “healthy eating”. Perhaps there is a true protective effect to eating red and processed meat as far as melanoma is concerned but this needs further study to confirm and understand. If confirmed understanding the mechanism may give insight into other ways of lowering melanoma risk that vegetarians can enjoy too.
Citation:
Red meat and processed meat intake and risk of cutaneous melanoma in white women and men: Two prospective cohort studies
Yen, Hsi et al.
Journal of the American Academy of Dermatology, 2018 In Press
Alzheimer’s or Skin Cancer?

What is the link between cancer and Alzheimer’s? A little know fact is that there seems to be a decreased risk of Alzheimer’s disease (a common form of dementia) in patients with various cancers. A recent study looked looked for this link with skin cancers and found a surprisingly large effect. Looking back at data from 82,925 patients aged 60 to 89 years old, researchers found the development of either melanoma or none melanoma skin cancer was associated with a significantly lower risk of subsequent Alzheimer’s disease. The mechanism for this “reverse association” is not clear, but hopefully further research may help elucidate more about the development of Alzheimer’s and ultimately may lead to strategies to decrease the risk of Alzheimer’s while avoiding the development of skin cancer.
Article Citation
Inverse Association for Diagnosis of Alzheimer’s Disease Subsequent to Both Melanoma and Non-Melanoma Skin Cancers in a Large, Urban, Single-Centre, Midwestern US Patient Population
J Eur Acad Dermatol Venereol 2018 Mar 24;[EPub Ahead of Print], E Ibler, G Tran, KA Orrell, L Serrano, S Majewski, KA Sable, R Thiede, AE Laumann, DP West, B Nardone
Dermatologists do it better!

When concerned about the possibility of skin cancer often the dermatologist can reassure the patient that the lesion is not worrisome, and save the patient the anxiety, scar and cost associated with a biopsy. However sometimes the lesion will be deemed suspicious enough to warrant a biopsy. There is both science and judgment involved in determining which lesions should or should not be biopsied. It is a skill that comes with knowledge, training and experience. A recent study has confirmed how difficult it is to avoid biopsying too much without at the same time missing something important. A study published in JAMA Dermatology found that dermatologist were on average more expert at this process than physican assistants (PAs). PAs required significantly more biopsies per melanoma discovered than dermatologists. But perhaps even more importantly, patients screened by a physician assistant were significantly less likely than those screened by a dermatologist to be diagnosed with melanoma in situ (the earliest stage of melanoma). The expert eye of a dermatologist can make a difference in saving a patient from an unnecessary biopsy and also picking up and early melanoma that might otherwise be missed.
Citation:
Accuracy of Skin Cancer Diagnosis by Physician Assistants Compared With Dermatologists in a Large Health Care System
Alyce M. Anderson, PhD1; Martha Matsumoto, MD2; Melissa I. Saul, MS3; et al Aaron M. Secrest, MD, PhD4,5; Laura K. Ferris, MD, PhD2
JAMA Dermatol. Published online April 18, 2018.
Skin Cancer Screen Exams Matter.
You may have expected it, but now its confirmed, having a full body skin cancer screening exam by a physician increases the chances of detecting an early rather than late melanoma. But what you may not have realized is the power of your own “self exam”. By performing regular self exams patients can increase the chances that any melanoma they develop will be detected earlier and thinner and so more likely curable. So get checked routinely but also make a habit of checking your own skin.
If you notice a suspect mole on your skin, you should follow the simple ABCDE rule which outlines the common warning signs of melanoma:
- Asymmetry: One half does not match the other half.
- Border irregularity: The edges are ragged, notched or blurred.
- Color: The pigmentation is not uniform. Shades of tan, brown or black are present. Occasionally dashes of red, white, and blue add to the mottled appearance.
- Diameter: The width is greater than six millimeters (about the size of a pencil eraser).
- Evolution: Any change or growth of a mole should be of concern.
And the “Ugly Duckling Rule”. : Look for the mole that stands out compared to your other moles.
Citation
Association of Skin Examination Behaviors and Thinner Nodular vs Superficial Spreading Melanoma at Diagnosis
Clio Dessinioti, MD
et al.
JAMA Dermatol. Published online April 18, 2018. doi:10.1001/jamadermatol.2018.0288
Marriage and Melanoma

Marriage just may save you from having a more advanced melanoma! A study from the University of Pennsylvania looked back at the marital status of over 50,000 patients diagnosed with melanoma. Married patients were more likely to be diagnosed with an earlier rather than latter stage of melanoma compared to none married patients. Earlier stages of melanoma have a higher cure rate and so it may be that being married is saving lives! The lowest risk for having a more advanced melanoma at diagnosis was for married patients, next, never married then divorced and highest risk was “never married”. The obvious thought would be having someone see your skin ever day will increase the likely-hood of a suspicious lesion being noticed, but it may also be that a concerned spouse is pushing reluctant patients to seek care earlier. Married or not, check your skin regularly and have any changing moles examined.
Citation:
Association of Marital Status With T Stage at Presentation and Management of Early-Stage Melanoma
Cimarron E. Sharon, BS1; Andrew J. Sinnamon, MD1; Michael E. Ming, MD, MSCE2; et alEmily Y. Chu, MD,
JAMA Dermatol. Published online April 18, 2018.
BRCA affects men too!
When most of us think of the BRCA 1 and BRCA 2 mutations we think of women and breast cancer. However BRCA mutations can increase the risk of other malignancies including melanoma. A recent study from Israel has show that men with these mutations are also at risk. They found that men with BRCA 1 or BRCA 2 mutations were at increased risk of melanoma and pancreatic cancer as well as breast cancer, (yes men can get breast cancer too!), and unique to men is an increased risk of prostate cancer. They recommend that men with these mutations get screened for prostate cancer and that both men and women with these mutations get screened for breast and pancreatic cancer as well as melanoma.
Citation:
In one year over 50% of young adults get a sunburn!

A study from from the CDC in Atlanta examined the prevalence of sun protection use and sunburn in a 31,162 U.S. adults in 2015.
The researchers found that 34.2 % of participants experienced sunburn in 2015. The prevalence was higher among younger age groups with 51.2 % of those aged 18 to 29 years experiencing a sunburn that year.
We know that sunburns are a significant risk factor for subsequent skin cancers. As dermatologist we are clearly not doing a good enough job getting the message out. We need to better educate our youth about the risks of “unprotected sun”. Its not just to pain a discomfort of the burn itself you want to avoid but the increased risk of a skin cancer in your future.
Start educating your kids early and be a good role model with your own sun protective practices.
Article Citation:
Prevalence of Sun Protection Use and Sunburn and Association of Demographic and
Behaviorial Characteristics With Sunburn Among US Adults
Dawn M. Holman, MPH1; Helen Ding, MD, MSPH2; Gery P. Guy Jr, PhD, MPH1; et alMeg Watson, MPH1; Anne M. Hartman, MS, MA3; Frank M. Perna, EdD, PhD3
JAMA Dermatol. Published online March 14, 2018. doi:10.1001/jamadermatol.2018.0028
