Cosmetic Surgery Blog
Understanding the Risks of a Second Melanoma

Melanoma is a serious form of skin cancer that arises from the pigment-containing cells known as melanocytes. While the initial diagnosis of melanoma can be daunting, a recent study from Norway sheds light on the increased risk of developing a second primary invasive melanoma, distinct from the first occurrence.
This finding emphasizes the need for ongoing vigilance and regular skin examinations for individuals who have previously been diagnosed with melanoma.
The Study’s Findings
Research conducted in Norway and published in JAMA Dermatology highlights a critical concern for melanoma patients: the significant risk of facing a second melanoma diagnosis, which is independent of the first.
This extensive study reveals that the likelihood of developing a second melanoma is notably higher in older patients and men. Nevertheless, it’s crucial for all melanoma patients, regardless of age or gender, to understand their heightened risk and take proactive steps toward skin health.
Why This Matters
The discovery of an increased risk for a second melanoma underlines the importance of diligent skincare and regular monitoring for all melanoma survivors. Melanomas can be effectively treated when caught early, making regular skin examinations a key component of post-diagnosis care. The findings from the study are an important reminder of the persistent vulnerability of melanoma patients to further skin cancers.
Recommendations for Melanoma Survivors
Given the elevated risk of subsequent melanoma, individuals with a history of melanoma should undergo comprehensive skin cancer screening exams. Initially, these should be conducted every three months for the first two years following a diagnosis.
After this period, the frequency of exams can be reduced to every six months. This schedule aims to ensure that any new melanomas are detected as early as possible, enhancing the effectiveness of treatment and improving outcomes.
The Importance of Skin Cancer Screening
Skin cancer screening involves a thorough examination of the skin for any signs of melanoma or other skin cancers. Dermatologists use a variety of tools and techniques to inspect moles, blemishes, and lesions for characteristics indicative of cancer. Early detection through these screenings is crucial, as it significantly increases the chances of successful treatment.
Taking Action
For those who have been diagnosed with melanoma, this study underscores the necessity of remaining vigilant about skin health and adhering to recommended screening schedules. Regular follow-ups are essential to monitor for signs of a second melanoma and to receive timely treatment if needed.
If you or someone you know has been affected by melanoma, consider these findings as a call to action. Regular examinations are not just precautionary measures—they are vital steps in safeguarding your health and well-being.
Schedule Your Consultation
Dr. Ralph Massey is committed to providing comprehensive care and support for individuals at risk of or diagnosed with melanoma in Santa Monica. He is a cosmetic and skin cancer surgeon who is fellowship-trained and board-certified in micrographic dermatologic surgery. Contact our practice today to schedule your consultation and take an important step toward proactive skin cancer prevention and care.
The Risks of General Anesthesia and 3 Alternatives to Sedation

General anesthesia is often the standard and only choice for pain-free and unconscious states during procedures. But as Dr. Ralph A. Massey prioritizes patient safety and education, patients need to be well-informed about the inherent risks linked to general anesthesia while learning about alternative methods that might present less risk, especially for specific types of surgery.
5 Risks Associated with General Anesthesia
While patients generally don’t have problems with general anesthesia, there are risks influenced by several factors including the patient’s overall health and age, the surgical procedure’s complexity, and the anesthesia’s duration. These might result in:
- Allergic Reactions: There is a potential for severe allergic reactions to anesthetic agents, which can lead to life-threatening conditions such as anaphylaxis. If you have sensitivities to any of these agents, bring this up during your consultation.
- Breathing Complications: Issues such as aspiration, where food or liquid is breathed into the lungs, or bronchospasm, a sudden constriction of the muscles in the walls of the bronchioles, are notable risks, impacting respiratory function.
- Cardiovascular Changes: The risk of experiencing significant fluctuations in blood pressure and heart rate during anesthesia is a concern, especially for those with existing cardiovascular conditions.
- Cognitive Effects: Postoperative confusion or cognitive dysfunction can be a significant concern for elderly patients, affecting their recovery and quality of life post-surgery.
- Nausea and Vomiting: Among the more common side effects, these can contribute to postoperative discomfort and potential dehydration, affecting the recovery process.
3 Alternatives to General Anesthesia
There are three known alternatives to general anesthesia, and they provide numerous benefits, including quicker recovery times, reduced risk of anesthesia-related complications, and the choice for patients to remain conscious if preferred.
1. Local Anesthesia
Local anesthesia works by temporarily blocking nerve signals in a specific area of the body, allowing the patient to remain fully awake and aware without feeling pain in the area being treated. Local anesthetics are commonly used for minor surgeries and procedures, such as dental work, skin biopsies, and some types of cosmetic surgeries.
The primary advantage of local anesthesia is its safety profile. Since the anesthetic effect is localized, it reduces the risk of several side effects and complications associated with general anesthesia. Recovery from local anesthesia is generally quick, with patients often able to resume their daily activities shortly after the procedure–with some pain medications.
2. Regional Anesthesia
Regional anesthesia involves numbing a larger portion of the body and can be divided into several types, including spinal, epidural, and nerve blocks. This method is particularly beneficial for procedures on the lower body, such as hip or knee surgery, and for pain management during childbirth.
This alternative allows patients to avoid the side effects and risks of general anesthesia while remaining comfortable during surgery. Additionally, it can offer pain relief for several hours or even days after the procedure, aiding in a smoother recovery process.
In our practice, we use nerve blocks to target specific nerve clusters to numb a particular body region during various procedures, including shoulder, arm, and leg surgeries.
3. Conscious Sedation
Conscious sedation, also known as procedural sedation or twilight sedation, provides a way for patients to be relaxed and comfortable during a procedure without being put into a deep sleep.
Conscious sedation offers several benefits, including reduced anxiety for the patient, decreased pain perception, and the ability to recover more quickly from the sedative effects compared to general anesthesia. It’s also known for its flexibility–being adjustable to suit the patient’s needs and the nature of the procedure.
Make the Right Decision with Dr. Massey
For individuals contemplating surgery and seeking to understand more about anesthesia options, including alternatives to general anesthesia, reach out to Dr. Ralph A. Massey’s practice today. Dr. Massey and his team in Santa Monica are committed to providing all the information you need to have the best surgical plan. Schedule a consultation today to make the right decision for your future procedure.
Understanding the ABCDEs of Melanoma
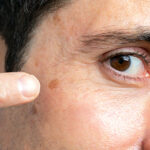
Cosmetic and skin cancer surgeon Dr. Ralph Massey specializes in the diagnosis and surgical treatment of melanoma in Santa Monica, CA. Dr. Massey is a tireless educator and advocate of the vital importance of detecting skin cancer early, especially if melanoma is suspected. Join us for the following insights from Dr. Massey on the ABCDEs of melanoma, a critical tool for helping in the early recognition of this most serious form of skin cancer.
The ABCDEs of Melanoma Explained
Melanoma is a formidable adversary, but knowledge is our greatest weapon in the fight against this condition. The ABCDEs of melanoma represent key characteristics of moles or growths that could signify the presence of cancer. Dr. Massey stresses the importance of familiarizing oneself with these signs:
Asymmetry – One-half of the mole or birthmark does not match the other. Healthy moles are typically symmetrical, so any asymmetry warrants closer examination.
Border – Irregular, scalloped, or poorly defined borders in a mole can be a warning sign. Unlike benign moles that have smoother, more even borders, malignant ones often display uneven edges.
Color – The presence of varied colors within a single growth – including shades of brown, black, pink, red, white, or blue – can indicate melanoma. Uniform coloration is more common in non-cancerous moles.
Diameter – Melanomas usually are larger in diameter than a pencil eraser (6mm). However, they can be smaller when first detected, making it crucial not to overlook smaller suspicious moles.
Evolving: Any change in size, shape, color, elevation, or another trait, or any new symptom such as bleeding, itching, or crusting, points to evolution. A mole that changes over time is a red flag.
Skin Cancer: The Importance of Early Detection
Early detection of melanoma can significantly enhance treatment success. Regular self-examinations using the ABCDE guide and annual skin checks by a dermatologist are vital strategies in identifying melanomas at their most treatable stage.
Preventing Skin Cancer: Sunscreen, Lifestyle and Diet can Minimize Risk
The importance of using a proper sunscreen to protect your skin from exposure to Ultra-Violet (U.V.) Light exposure can not be overstated. Whether from the sun or tanning beds, U.V. Light is a known carcinogen that causes the majority of skin cancers. Applying broad-spectrum sunscreen of SPF 30 or higher every two to three hours and wearing protective clothing can significantly minimize the risk for developing melanoma.
While avoiding sun exposure during peak hours and the diligent use protective clothing and sunscreen are the first lines of defense against developing skin cancer, following are some additional preventative measures to consider:
Oral vitamin D supplements – For individuals seeking the therapeutic benefits of the sun or tanning booths, vitamin d supplements have been shown to provide similar benefits in place of sun exposure and the use of tanning beds.therapeutic benefits in place of sun exposure or the use of tanning beds.
Nicotinamide (Vitamin B3) – High-risk individuals can reduce their risk of basal cell and squamous cell skin cancers by over 20% through the twice-daily oral intake of 500 mg nicotinamide (vitamin B3). This readily available supplement is considered safe.
Low Fat Diet – Evidence suggests that maintaining a low-fat diet (less than 20% of calories from fat) over the long term may lower the risk of skin cancer.
Tea Consumption – Incorporating black or green tea into daily consumption habits may slightly reduce the long-term risk of skin cancer.
Skin Resurfacing – Procedures such as CO2 laser or medium-depth chemical peels offer dual benefits: they improve skin appearance while also reducing the risk of further skin cancers in treated areas by addressing sun damage.
DNA Repair Enzymes – To mitigate UV-induced damage and reduce the risk of skin cancer, topical DNA repair enzymes can be utilized. Eryfotona Actinic sunscreen contains these enzymes.
Aspirin and Melanoma – Studies suggest that daily aspirin intake may decrease the risk of melanoma in women, although this effect has not been observed in men. Further research is necessary to fully understand this relationship.
Antihistamines – While preliminary evidence suggests that daily use of the oral antihistamine desloratadine (Clarinex) may slightly lower the risk of melanoma, further research is needed for confirmation.
Expertise in Treatment
Dr. Massey is fellowship-trained in a procedure called Mohs micrographic surgery. This precise surgical technique first involves the removal of unhealthy tissue structures that rise above the skin’s surface. The next stage of the surgery continues with the removal and evaluation of microscopic layers of skin tissue lying underneath and in tissue margins around the removed growth. This meticulous process continues until examination of a removed layer confirms that no cancerous or precancerous cells remain.
Mohs surgery is highly effective in removing unhealthy cells while preserving as much healthy tissue as possible to aid in cosmetic reconstruction. As a leader in both cosmetic and cancer surgery, Dr. Massey leverages his extensive skill set to not only treat skin cancer effectively but also to restore and enhance his patients’ appearance post-surgery.
Contact Our Office
Contact us to schedule a skin cancer consultation with Dr. Massey in Santa Monica, our practice provides patients with the comfort and convenience of an on-site surgical suite and diagnostic lab. The doctor’s commitment to patient education, along with his comprehensive approach to skin cancer treatment, makes him a trusted ally in the fight against skin cancer.
Beyond Beauty: The Unexpected Health Benefits of Cosmetic Surgery

Cosmetic surgery has always been synonymous with enhancing beauty and aesthetics. Patients often choose cosmetic surgery primarily to enhance their physical appearance. However, its benefits extend far beyond aesthetics.
There are actually a number of health benefits provided by cosmetic surgery. Here at Ralph A. Massey Cosmetic & Skin Cancer Surgery, our priority is to provide not only aesthetic results but also consider the health benefits of cosmetic procedures in Santa Monica.
Physical Health Improvements
While cosmetic surgery mainly focuses on aesthetics, there are many cosmetic procedures that also address physical health concerns.
Take breast reduction, for example. This procedure addresses the chronic pain suffered by patients due to massive breast size weighing heavily on their shoulders and chest area. It also reduces rashes beneath the breasts, posture issues, and painful bra-strap indentations.
Another example is blepharoplasty surgery. By reducing the sagging of the upper eyelids, this procedure can effectively address obscured peripheral vision. This issue most frequently affects older patients.
Rhinoplasty is also performed for functional purposes. When a patient experiences breathing difficulties due to their nasal structure, functional rhinoplasty can be performed to clear the nasal passages.
Benefits of Cosmetic Surgery in Skin Cancer
Cosmetic surgery, especially when performed by an expert skin cancer surgeon like Ralph A. Massey, MD, can play a vital role in the recovery process for skin cancer patients.
Skin cancer removal can effectively get rid of cancer cells and prevent this issue from getting worse. However, this may result in a defect in the skin. To address this, Dr. Massey can provide reconstructive cosmetic procedures such as skin grafts, flap surgery, and scar revision.
These procedures help restore the natural appearance of the area and improve functional aspects such as mobility and comfort. Beyond aesthetics, these surgeries contribute to emotional healing, helping patients regain their sense of self.
Enhanced Confidence and Mental Wellbeing
Cosmetic procedures such as rhinoplasty, breast augmentation, and the buttocks lift are designed to specifically improve the physical appearance of a patient, and these changes can sometimes lead to increased confidence. Physical appearance may not be the sole basis for one’s self-esteem, but in some cases, it can play a major role in the level of confidence a person can experience. This newfound self-assuredness can lead to a more positive outlook on life and an improvement in mental wellbeing.
Enhanced Quality of Life
Cosmetic surgery can allow patients to feel more comfortable at social gatherings, in the workplace, and during intimate moments. This will allow them to lead fuller, more satisfying lives by reducing self-consciousness during interactions.
Improved Social and Professional Opportunities
A more attractive appearance can create opportunities in both social and professional settings. Individuals who feel good about their appearance tend to be more self-assured during job interviews and social gatherings. This can lead to more fulfilling social relationships and better career opportunities. Individuals with increased confidence can perform better at work and be more successful at networking.
Take the First Step Towards Transformation
Cosmetic surgery can extend beyond beauty, impacting physical health and wellbeing. If you’re considering cosmetic procedures in Santa Monica, there’s no better partner on this journey than Ralph A. Massey MD Cosmetic & Skin Cancer Surgery.
We understand the profound impact that the right cosmetic procedures can have on your life. With his expertise in both cosmetic and skin cancer surgery, Dr. Massey is the ideal choice for your next procedure. Contact us today to schedule an appointment and begin your transformation!
Protect your Children from Sunburns
The association between sun exposure and skin cancer has become more widely understood over the years as studies and research continue to be done.
In a recent cohort study, the long-term risk of developing skin cancer as a result of sunburns has been confirmed. The study used information gathered between 1991 to 2007 through a baseline questionnaire that included questions about the number of sunburns experienced. Follow-up questionnaires were answered every five to seven years. The data for this study was gathered by the Norwegian Women and Cancer Study which was established in 1991.
The analysis of the data from the study showed that those who experienced a high frequency of sunburns throughout their lives had a notably increased risk of developing cutaneous squamous cell carcinoma and melanoma. The data also showed that those who frequently experienced sunburns during childhood had an even higher risk of developing these skin cancers. The research indicates that properly protecting yourself from the sun and avoiding sunburns, especially during childhood, is incredibly important when it comes to reducing the risk of skin cancer.
Article Citation:
Lifetime Sunburn Trajectories and Associated Risks of Cutaneous Melanoma and Squamous Cell Carcinoma Among a Cohort of Norwegian Women Simon Lergenmuller, PhD1,2; Corina S. Rueegg, PhD3; Flavie Perrier, PhD1; et alTrude E. Robsahm, PhD4; Adele C. Green, PhD5,6; Eiliv Lund, PhD4,7; Reza Ghiasvand, PhD3,4; Marit B. Veierød, PhD1
JAMA Dermatol. Published online October 5, 2022. doi:10.1001/jamadermatol.2022.4053
How Alcohol Consumption May Increase Your Risk of Melanoma

The link between alcohol consumption and an increased risk of melanoma can be attributed to multiple factors according to recent studies. While other studies have indicated that alcohol consumption increases the risk of sunburn due to ineffective sunscreen application and prolonged sun exposure, Dermatologist Dr. Niyati Sharma has noted that a German study has also found that alcohol consumption has also been linked to increased severity of sunburns.
One study has shown a 7% increase in the risk of basal cell carcinoma and an 11% increase in the risk of squamous cell carcinoma for every standard-sized beer, small glass of wine, or 10g of distilled spirit consumed daily. Another study also found that there was a 20% increase in the risk of melanoma in those who consumed liquor compared to those who abstained or consumed alcohol infrequently. That number rose to 55% in those who consumed 50g of alcohol per day.
The exact cause of this increased risk is not known yet, but Dr. Sharma has noted that a lower level of carotenoids in those who consume alcohol is likely the cause of increased sensitivity to developing more severe sunburns at an accelerated rate.
Mohs proves itself better again, even in Desmoplastic Melanoma!
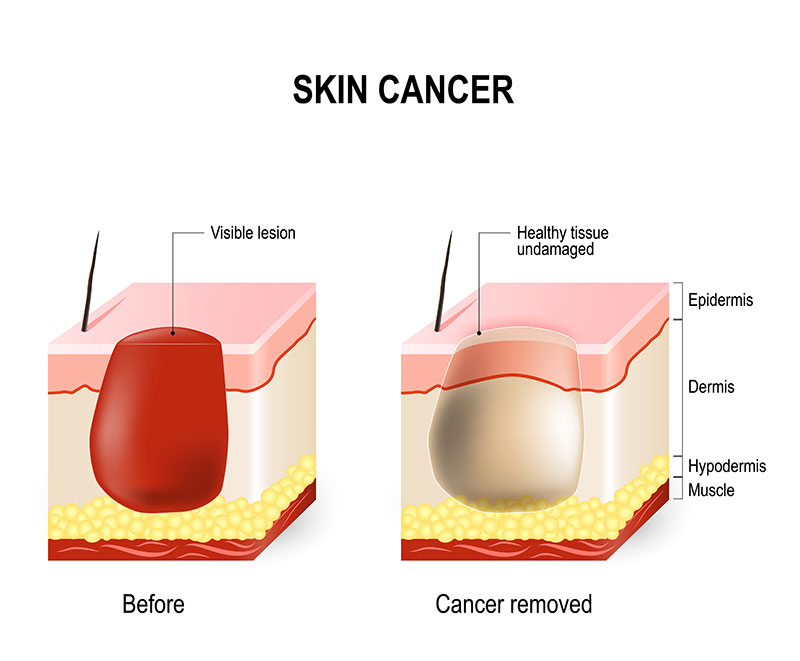 Mohs surgery is a procedure used to treat skin cancer. This surgery removes a narrow margin of normal looking skin beyond the obvious tumor. This tissue is processed in such a way that all of the outer margin and underside can be examined under the microscope. If residual cancer is seen reaching the outer edges a further thin margin is removed in that area only. The process is repeated until all the margins are proved to be clear.
Mohs surgery is a procedure used to treat skin cancer. This surgery removes a narrow margin of normal looking skin beyond the obvious tumor. This tissue is processed in such a way that all of the outer margin and underside can be examined under the microscope. If residual cancer is seen reaching the outer edges a further thin margin is removed in that area only. The process is repeated until all the margins are proved to be clear.
Desmoplastic melanoma is a dangerous form of melanoma with a particularly high rate of local recurrence after standard surgical excision. While there have been previous studies showing Mohs surgery to be equal or better than regular wide excision for early regular melanomas, this is the first study indicating Mohs surgery also gives an advantage over wide surgical excision for desmoplastic melanoma as well.
In this retrospective single-institution study of 109 desmoplastic melanoma cases, 63 were treated with wide local excision (WLE) and 46 were treated with Mohs micrographic surgery (MMS). The local recurrence rate for WLE was 8%, and 11% of the patients required repeat surgery for local recurrence or positive/equivocal margins after WLE. No local recurrence was reported among patients treated with MMS; however, 1 patient required repeat surgery due to positive margins observed on permanent frozen sections.
Melanoma, Skin Cancer Screenings, and Early Detection
Skin cancer is the most common type of cancer by a wide margin. There is a variety of different types of skin cancers that someone may develop at some point in their life. One of the most concerning types of skin cancer is melanoma.
Like other forms of cancer, melanoma forms when the cells in the body grow into a mass of cancerous cells. In the case of melanoma, the cells that are affected are the melanocytes, the pigment-producing cells responsible for producing melanin, which gives the skin a tan or darker color.
Melanomas can form on any area of the body, though they most commonly form in areas like the face, back, legs, arms, and other places that are frequently exposed to sunlight. They can also form on areas that do not receive large amount of sunlight, like the soles of the feet and the palms of the hands.
Symptoms and Signs of Melanoma
Some of the most common early signs of melanoma are a new dark spot on the skin or a noticeable change in an existing mole. These changes can pertain to the shape, size, or color of the dark spot or mole. Another indication could be a mole or dark spot that has a noticeably different appearance compared to others on the skin.
Other signs to look out for include an irregular border around the mole or dark spot, changing colors within the same mole, changes in shape and color over time, and asymmetry between different halves of a singular mole or dark spot.
The Importance of Regular Screenings for Melanoma
When it comes to treating melanoma, early detection is essential. If melanoma is caught early, the chance of successfully curing it is significantly higher. Some people also have a higher risk of developing melanoma, which makes early detection and regular screening for melanoma very important.
Just how important are regular screenings for melanoma? A study recently published in The British Journal of Dermatology studied 43,762 residents of Queensland, Australia, who were within the age range where the chance of developing melanoma was high. The study identified those who had undergone a skin cancer screening prior to the baseline set at the start of the study. Participants were also asked to fill out a comprehensive melanoma risk factors survey.
During the study, researchers calculated the incidence of confirmed melanoma cases among the patients being studied between the second and seventh years of the study. Researchers then measured the rate of biopsies performed amongst these patients between the second and sixth years of the study.
Once concluded, the study found that there was a clear higher rate of early detection in patients who underwent skin cancer screenings and a higher rate of biopsy in those patients. It should be noted that some of the melanomas discovered and treated through these screenings may have been indolent with a low chance of leading to death.
Taking the Steps to Protect Yourself
Whether you have a high risk of developing a melanoma or you just want to make sure that your skin and body are as healthy as possible, regular skin cancer screenings performed by a skin cancer expert are important for early detection. Dr. Massey is a renowned cosmetic and skin cancer surgeon who is dedicated to helping keep all of our patients safe and healthy. Contact our office today to schedule your skin cancer screening.
Protected: Delays in Surgical Treatment of Melanoma and Mortality
The Perils of Biotin Supplementation
This is an important note to all of my patients because of the frequency of biotin use by the public. Many doctors have recommended biotin as a supplement for years as it is inexpensive and easy to use. It is a water-soluble vitamin, which while it does little harm, the therapeutic benefit is negligible and it can contaminate lab test results (see the list below). In addition, there are no easy fixes for many of the nail and hair problems that Biotin may be recommended to help.
The lab test interference goes beyond troponin and thyroid tests. This list is likely to grow. In light of this it is now generally recommended to stop biotin 2 days before getting any blood work done.
Lab tests affected by biotin supplementation
- Thyroid
- Troponin (58.6%)
- 25-Hydroxy vitamin D
- Beta-human chorionic gonadotropin
- Hepatitis
- Human immunodeficiency virus serology
Article Citation:
Journal of the American Academy of Dermatology
Biotin Beware: Perils of Biotin Supplementation
J Am Acad Dermatol 2022 Feb 24;[EPub Ahead of Print], JM Falotico, SR Lipner
