Melanoma
Ralph A. Massey, MD — Santa Monica & Encino, CA

-
What is melanoma?
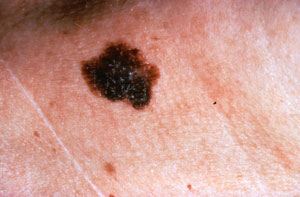 A melanoma is a type of skin cancer. It is characterized by the uncontrolled growth of “melanocytes”, pigment-producing tanning cells. Melanomas may suddenly appear without warning, but can also develop from a preexisting mole. They are found most frequently on the sun-exposed areas, but can occur anywhere on the body.
The overall incidence of melanoma is rising at an alarming rate. At current rates one in 65 Americans have a lifetime risk of developing invasive melanoma, a 2000% increase from 1930. (In addition, with the inclusion of the earliest stages of melanoma, melanoma in situ, one in 37 Americans have a lifetime risk of developing melanoma!)
A melanoma is a type of skin cancer. It is characterized by the uncontrolled growth of “melanocytes”, pigment-producing tanning cells. Melanomas may suddenly appear without warning, but can also develop from a preexisting mole. They are found most frequently on the sun-exposed areas, but can occur anywhere on the body.
The overall incidence of melanoma is rising at an alarming rate. At current rates one in 65 Americans have a lifetime risk of developing invasive melanoma, a 2000% increase from 1930. (In addition, with the inclusion of the earliest stages of melanoma, melanoma in situ, one in 37 Americans have a lifetime risk of developing melanoma!)
-
Is melanoma a serious disease?Melanoma can spread to internal organs and may result in death. One person each hour dies from melanoma in the U.S.. However, if detected in the early stages, melanoma can usually be treated successfully.
-
What causes melanoma?While not all melanomas are sun related, excessive exposure to ultraviolet radiation from the sun is the most important preventable cause of melanoma. People in southern regions, where the sunlight is more intense, are more likely to develop melanoma than those in northern regions. Melanoma has been particularly linked to excessive sun exposure in the first 10 to 18 years of life. Other possible factors include genetic factors and immune system deficiencies.
-
Who gets melanoma?Melanoma can strike anyone. However, Caucasians are ten times more likely to be diagnosed with melanoma than other races. Even among Caucasians, certain individuals are at higher risk than others. For example:
- Your chances increase significantly if you’ve already had one melanoma.
- You have a substantially increased risk of developing melanoma if you have many moles, large moles or atypical (unusual) moles.
- Your risk is increased if your parents, children or siblings have had melanoma.
- If you are a Caucasian with fair skin, your risk is four times as great as a Caucasian with olive skin.
- Redheads and blondes have a twofold to fourfold increased risk of developing melanoma.
- Excessive sun exposure in the first 10 to 18 years of life increases your chances of developing melanoma.
-
What are atypical moles?Most people have moles (also known as nevi). Atypical moles are unusual moles that are generally larger than normal moles, variable in color, often have irregular borders and may occur in far greater number than regular moles. Atypical moles occur most often on the back and also commonly occur on the chest, abdomen and legs in women. It is important to recognize that atypical moles are not limited to any specific body area — they may occur anywhere. The presence of multiple atypical moles may mark a greater risk of melanoma developing either in a mole or on apparently normal skin.
-
What does melanoma look like?
Recognition of changes in the skin is the best way to detect early melanoma. Melanoma generally begins as a mottled, light brown to black flat blemish with irregular borders. Occasionally, it may turn shades of red, blue or white, crust on the surface and bleed. They most frequently appear on the upper back, torso, lower legs, head and neck. A changing mole, a new mole, or a mole that is different or “ugly” or begins to grow should be examined carefully. If you notice a mole on your skin, you should follow the simple ABCDE rule which outlines the warning signs of melanoma: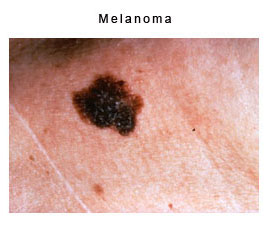
- Asymmetry: One half does not match the other half.
- Border irregularity: The edges are ragged, notched or blurred.
- Color: The pigmentation is not uniform. Shades of tan, brown or black are present. Occasionally dashes of red, white, and blue add to the mottled appearance.
- Diameter: The width is greater than six millimeters (about the size of a pencil eraser).
- Evolution: Any change or growth of a mole should be of concern.
-
Can melanoma be cured?When detected in its earliest stages, melanoma is highly curable. The average five-year survival rate for individuals with melanoma is 89 percent. For localized melanoma, melanoma that has not spread beyond the outer layers of the skin at the time of detection, the average five-year survival rate is 96 percent. Approximately 82 percent of melanomas are diagnosed at a localized stage.* When detected early, surgical removal of thin melanomas can cure the disease in most cases. Early detection is essential; there is a direct correlation between the thickness of the melanoma and survival rate. We recommend a regular self-examination of the skin to detect changes in its appearance. Additionally, patients with risk factors should have a complete skin examination by a dermatologist annually. Patients with a history of skin cancer need more frequent checks. To assist with monitoring full body photographic mole mapping is recommended.
-
Can melanoma be prevented?Because overexposure to ultraviolet light is thought to be a primary cause of many melanomas, we recommend the following precautions:
- Avoid “peak” sunlight hours — 10 a.m. until 4 p.m. — when the sun’s rays are the strongest.
- Seek shade whenever possible. Remember “No shadow, seek the shade!” If your shadow is shorter than you are, the damaging rays of the sun are at their strongest and you’re likely to sunburn.
- Wear protective clothing, including a wide-brimmed hat, sunglasses and long-sleeved shirt and pants during prolonged periods of sun exposure.
- Apply a broad spectrum sunscreen with a Sun Protection Factor (SPF) 15 or higher, 15 – 30 minutes before going outdoors and reapply every two hours, especially when involved in outdoor activities such as gardening or swimming.
- Some recent studies have suggested that long-term aspirin use may be associated with a reduced risk of melanoma, especially in women.
Prevention and Treatment
Prevention is an important way to combat all skin cancers. To learn more about skin cancer prevention, visit our prevention page. To learn more about the treatment of squamous cell skin cancer, visit our skin cancer treatment page.Your Melanoma will be performed by Dr. Ralph A. Massey himself, within his certified outpatient surgery center in Santa Monica.
“Truly greateful for the high quality of care”
Read full testimonial“so much expertise, caring and friendship”
Read full testimonial“What an amazing healer!”
Read full testimonial“Simply the best of the best”
Read full testimonial“This doctor walks on water”
Read full testimonial